Digestive symptoms should be a new focus for clinicians testing for novel coronavirus (COVID-19). Although most patients present with fever, dry cough, and dyspnea, the authors reported that patients do present with symptoms such as diarrhea, nausea, vomiting, and abdominal discomfort.
What are the symptoms?
Common symptoms are Abdominal pain, diarrhea, anorexia, and vomiting. Anorexia is more common and can be found in 80 % of patients. The average time from onset of symptom to hospital admission was 8.1 days. However, it was 9.0 days for patients with GI symptoms, including those with anorexia, compared with 7.3 days for those who did not have digestive symptoms.
The most important point to note is that few patients can have only digestive symptoms, but no respiratory symptoms at admission.
Can a virus have a fecal-oral route of transmission?
Yes. Investigators from Guangdong Province in China examined the viral RNA in the stool of 71 patients with confirmed COVID-19. The duration of positive stool tests may range from 1-to 12 days and patients can remain positive via stool tests after showing negative in respiratory samples.
Because COVID-19 is found in the stool, it’s probably best to use meticulous hand hygiene and bleach/antiseptic wipes in shared bathrooms (if self-quarantined).
Can this virus cause liver injury?
Yes. Mild to moderate liver injury as revealed by elevated aminotransferases, hypoproteinemia, and prothrombin time prolongation is described in these patients. However, there is not much data about this virus as a hepatotropic virus. Liver damage might be because of immune overreaction or antiviral use.
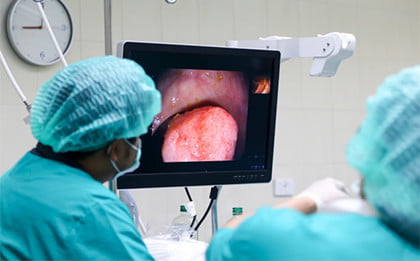
What is the evidence of Gastrointestinal tract involvement?
There is clear evidence from endoscopy that it can damage the stomach and the intestines. Patients with more gastric body involvement do have worse outcomes.
What is the outcome?
Patients with digestive symptoms have a longer time from onset of admission and their prognosis is worse than patients without digestive symptoms. The authors reported that 60% of patients without digestive symptoms recovered and were discharged, only 34.3% of the patients with digestive symptoms recovered.
Conclusion: Physicians should recognize that digestive symptoms may be a presenting feature of COVID-19, and there should be an increased index of suspicion for an early diagnosis than waiting for respiratory symptoms to develop. The virus has the potential for fecal-oral transmission.